Why Clinical Trials Have Specific Requirements (And What They Mean for You)
Clinical trial inclusion criteria determine who can participate in medical research. These requirements often frustrate people who want to join trials but don’t meet specific age ranges, lab values, disease stages, or health conditions.
Understanding why clinical trial inclusion criteria exist helps you recognize that these requirements protect both participant safety and scientific validity. They’re not arbitrary barriers designed to exclude people. They’re carefully designed parameters that ensure trials answer specific research questions accurately.

What Clinical Trial Inclusion Criteria Actually Are
Clinical trial inclusion criteria are the specific characteristics participants must have to qualify for a study. These requirements define the exact population researchers want to study.
Common Inclusion Criteria
Typical clinical trial inclusion criteria include:
- Age ranges like 18-65 years or 55 and older
- Specific diagnosis confirmed by particular tests
- Disease stage or severity measured by defined criteria
- Laboratory values within certain ranges
- Time since diagnosis such as within the past year
- Current treatment status including stable medication regimens
- Ability to complete study requirements like attend frequent visits
Each criterion serves a specific purpose in the research design. Nothing appears in inclusion criteria without reason.
Exclusion Criteria Work Together
Exclusion criteria list characteristics that disqualify people from participation. These work with inclusion criteria to define exactly who should and shouldn’t participate.
Common exclusions include:
- Pregnancy or breastfeeding
- Certain medications that might interfere with the study drug
- Other health conditions that could complicate results
- Recent participation in other trials
- Inability to provide informed consent
Together, clinical trial inclusion criteria and exclusion criteria create a precise definition of eligible participants.

Why Age Requirements Exist
Age restrictions in clinical trial inclusion criteria frustrate many potential participants. Understanding the reasons helps you evaluate whether these requirements make sense for specific studies.
Physiological Differences by Age
Bodies process medications differently across age groups. Metabolism slows with age. Kidney and liver function change. Drug interactions vary based on how many medications someone takes, which increases with age.
When researchers test a new treatment, they need to control these variables. Starting with a specific age range lets them understand how the drug works in that population before expanding to other ages.
Pediatric Protections
Children receive extra protection in research. Trials involving minors require additional ethical oversight. Researchers must justify why children are necessary for the study and demonstrate that adult trials wouldn’t provide the needed information.
This is why many clinical trial inclusion criteria specify adults only. It’s not that researchers don’t care about pediatric applications. It’s that testing in children requires different protocols and additional safeguards.
Testing Across Age Groups
After establishing safety in one age group, researchers expand to others. A medication tested in adults 18-65 might later be studied in people over 65, then eventually in adolescents and children if appropriate.
This staged approach protects each population while systematically gathering data about how treatments work across ages.

Disease Stage Requirements
Clinical trial inclusion criteria often specify exact disease stages. This requirement reflects what the trial is designed to test.
Early-Stage Trials Need Early-Stage Disease
Trials testing whether early treatment prevents disease progression need participants with early-stage disease. Including people with advanced disease would prevent researchers from answering whether early intervention works.
If clinical trial inclusion criteria require recent diagnosis or mild disease, it’s because the research question specifically asks whether treating early makes a difference.
Advanced Disease Trials
Conversely, some trials test treatments for advanced disease that hasn’t responded to standard options. These trials need people with specific disease characteristics that define “advanced” or “refractory.”
Clinical trial inclusion criteria for these studies exclude people with mild disease because the treatment being tested might be too aggressive for early stages. Researchers need data about whether strong interventions help when gentler approaches have failed.
Why Mixing Stages Creates Problems
Including participants across all disease stages in one trial makes results difficult to interpret. If a treatment works for early-stage but not advanced disease, combining all participants might show no overall benefit, missing the early-stage effectiveness.
Specific clinical trial inclusion criteria by disease stage let researchers understand exactly when and for whom treatments work.

Laboratory Value Requirements
Many clinical trial inclusion criteria specify particular lab values. These requirements protect safety and ensure participants can demonstrate whether treatments work.
Safety Thresholds
Some lab values indicate whether your body can safely process the study medication. Kidney function tests show whether your kidneys can filter the drug. Liver function tests reveal whether your liver can metabolize it.
If clinical trial inclusion criteria require specific kidney or liver values, it’s because the study drug might be dangerous for people whose organs aren’t functioning adequately.
Measuring Treatment Effect
Other lab values provide baseline measurements that researchers will track throughout the trial. For diabetes trials, hemoglobin A1c must be high enough to show whether treatment improves it. For cholesterol trials, LDL levels must be elevated enough to demonstrate reduction.
If you meet the lab requirements too well because your current treatment is highly effective, adding a new medication might not show benefit. This doesn’t mean the new treatment doesn’t work. It means your labs don’t leave room to demonstrate improvement.
Creating Comparable Groups
Clinical trial inclusion criteria specifying lab ranges create participant groups that are similar to each other. This comparability makes it easier to determine whether observed differences come from the treatment rather than underlying health variations.

Previous Treatment Requirements
Clinical trial inclusion criteria often specify what treatments you’ve tried before or what medications you’re currently taking.
Treatment-Naive Trials
Some trials want “treatment-naive” participants who haven’t tried standard medications yet. These trials test whether new treatments work as first-line therapy.
Clinical trial inclusion criteria for treatment-naive studies ensure participants haven’t already responded well to existing options, which would make it hard to show whether the new treatment adds value.
Treatment-Resistant Trials
Other trials specifically need people whose current treatment isn’t working. These studies test whether new medications help when standard options fail.
If clinical trial inclusion criteria require that you’ve tried and failed multiple treatments, the trial is investigating whether the new option works for treatment-resistant disease.
Stable Medication Requirements
Many clinical trial inclusion criteria require stable medication regimens, meaning your doses haven’t changed recently. This stability creates a consistent baseline for measuring new treatment effects.
If your medications are frequently adjusted because your condition is unstable, adding a study drug makes it impossible to determine what’s causing any changes observed.
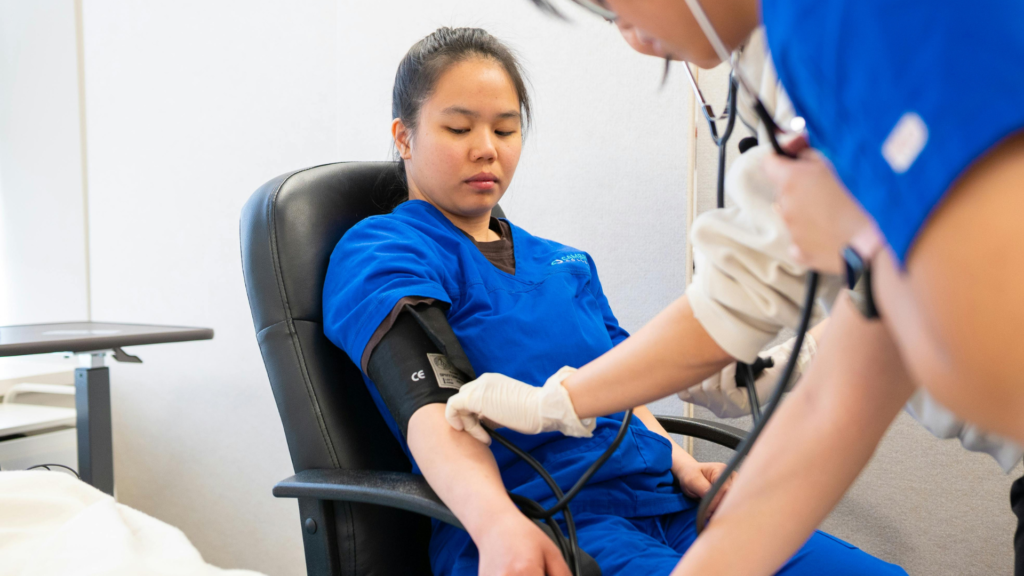
Practical Considerations
Clinical trial inclusion criteria also address practical factors that affect whether you can successfully participate.
Visit Schedule Requirements
Some clinical trial inclusion criteria specify that you must be able to attend visits at required frequencies. This isn’t arbitrary gatekeeping. If the protocol requires weekly visits for safety monitoring, enrolling someone who can’t attend weekly creates incomplete data and potential safety risks.
Transportation and Location
Trials conducted at specific sites might require that you live within a certain distance or have reliable transportation. This ensures you can attend all scheduled visits.
Some trials now offer virtual visits or home nursing, expanding clinical trial inclusion criteria to include people who couldn’t previously participate due to distance.
Language and Literacy Requirements
Informed consent requires that you understand what you’re agreeing to. Clinical trial inclusion criteria might specify language fluency or ability to complete written assessments in certain languages.
This reflects available resources at research sites, not intentional exclusion. Sites with bilingual staff can include non-English speakers in their clinical trial inclusion criteria.

Why You Might Not Qualify
Understanding clinical trial inclusion criteria helps you recognize that not qualifying doesn’t mean something is wrong with you or that researchers don’t care about people like you.
You’re Not the Target Population
If clinical trial inclusion criteria specify Type 2 diabetes and you have Type 1, you’re not excluded because researchers think you’re less important. You’re excluded because the trial tests treatments specifically for Type 2 diabetes that work differently than Type 1 treatments.
Different trials exist for different populations. Not qualifying for one doesn’t mean no trials need someone with your characteristics.
Safety Concerns
Sometimes clinical trial inclusion criteria exclude you because the study drug might be dangerous for people with your health characteristics. Being excluded protects you from potential harm.
This is particularly true for pregnancy exclusions. Most trials exclude pregnant women not because researchers don’t care about pregnant people, but because testing new drugs during pregnancy requires special protocols and ethical considerations.
Your Disease Is Too Controlled
If your condition is well-managed on current treatment, you might not qualify for trials testing new medications. This seems counterintuitive, but trials need to demonstrate that new treatments work.
If your labs are already normal and symptoms well-controlled, adding a new medication can’t show benefit because you’re already doing well.

What Inclusion Criteria Mean for Future Access
Clinical trial inclusion criteria affect not just who participates in trials, but who benefits from resulting treatments.
Tested Populations Get Approved Use
The FDA approves medications for populations studied in clinical trials. If trials only enrolled adults 18-65, initial approval might be limited to that age group. Expanding to other populations requires additional trials.
This is why diverse clinical trial inclusion criteria matter. Testing treatments in varied populations means broader approved uses when drugs reach the market.
Label Restrictions
When clinical trial inclusion criteria exclude certain groups, resulting drug labels might restrict use in those populations. Medications might have warnings about use in people with kidney disease if trials excluded people with poor kidney function.
This doesn’t necessarily mean the drug is dangerous for excluded groups. It means no data exists about safety and effectiveness in those populations.

Finding Trials That Match You
Rather than feeling frustrated by clinical trial inclusion criteria that exclude you, focus on finding trials where you match the target population.
Search Strategies
When searching ClinicalTrials.gov or other databases:
- Use filters for your specific condition and characteristics
- Read full eligibility criteria carefully before contacting sites
- Contact research coordinators with questions about borderline criteria
- Ask about upcoming trials if current ones don’t fit
Working with Research Coordinators
Research coordinators can help determine whether you meet clinical trial inclusion criteria. Sometimes criteria that seem disqualifying have flexibility. Lab values might have small windows. Recent diagnoses might have grace periods.
Don’t self-reject before discussing your situation with the research team. They can tell you definitively whether you qualify.
Multiple Trials Often Exist
If you don’t meet clinical trial inclusion criteria for one study, ask about others. Research sites often conduct multiple trials. You might not qualify for the diabetes trial requiring treatment failure but perfectly match the prevention trial needing people with pre-diabetes.

The Balance Between Inclusion and Science
Clinical trial inclusion criteria balance scientific validity with the goal of making research accessible. Overly restrictive criteria make enrollment difficult and limit how well results apply to real-world populations. Overly broad criteria create participant groups so diverse that results become difficult to interpret.
Researchers work to define clinical trial inclusion criteria that are specific enough for scientific rigor while inclusive enough to generate broadly applicable data. This balance isn’t perfect, but understanding the reasoning helps you evaluate whether specific requirements make sense.
What This Means for You
Clinical trial inclusion criteria shouldn’t discourage you from exploring trial participation. Instead, use them as guides to find studies that specifically need someone with your health characteristics.
At Valiance Clinical Research, we conduct trials across multiple conditions and disease stages. Our research coordinators help potential participants understand whether they meet specific clinical trial inclusion criteria. We explain why requirements exist and help you find trials that match your situation.
Clinical trial inclusion criteria exist to protect your safety and ensure research generates valid results. When you meet the requirements for a trial, you’re exactly the participant researchers need to answer important medical questions. When you don’t qualify, different trials exist that need someone with your characteristics. Understanding the requirements helps you navigate clinical research effectively.