Long-Term Follow-Up: The Commitment Behind Clinical Research Safety
Long-term follow-up clinical trials represent one of the most important yet least understood aspects of medical research safety. These studies continue monitoring participants for months, years, or even decades after active treatment ends to ensure a comprehensive understanding of how experimental therapies affect people over time.
Long-term follow-up clinical trials serve as essential safety nets that can detect delayed effects, late-onset side effects, or unexpected benefits that only become apparent with extended observation. This ongoing vigilance protects both current participants and future patients who might receive these treatments.
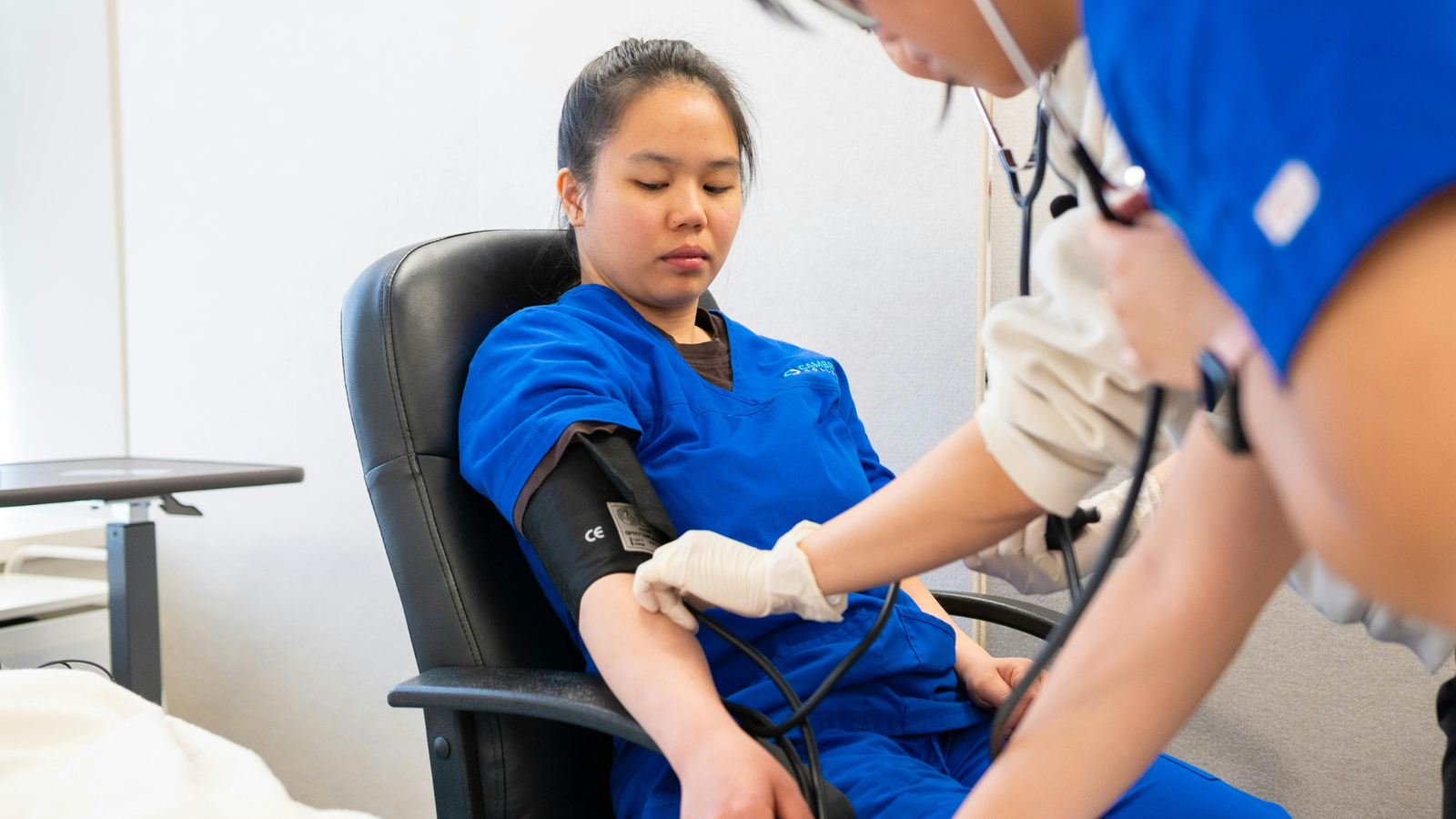
The Science Behind Long-Term Monitoring
Long-term follow-up clinical trials address fundamental biological realities about how treatments affect the human body over extended periods. Many medical interventions have effects that don’t become apparent immediately or that change over time.
Some treatments work by modifying cellular processes or genetic expression patterns that may have consequences years later. Cancer treatments, for example, might successfully eliminate tumors but potentially increase risks for different cancers decades in the future. Only long-term follow-up clinical trials can detect these delayed relationships.
Immune system modifications through treatments like immunotherapies or vaccines may have effects that evolve over the years. The immune system’s complexity means that beneficial or harmful changes might not stabilize immediately after treatment. Long-term follow-up clinical trials track these evolving immune responses.
Biological processes that require long-term monitoring include:
- Cellular damage that accumulates over time and leads to delayed complications
- Hormonal changes that affect multiple organ systems gradually
- Metabolic modifications that influence disease risk over the years
- Genetic or epigenetic changes that may affect future health outcomes
Drug metabolism and clearance patterns vary significantly between individuals. Some people eliminate medications quickly, while others process them slowly. These differences may lead to delayed effects that only become apparent through long-term follow-up clinical trials involving diverse populations.
Age-related factors influence how treatments affect people over time. Treatments received in youth may have different long-term consequences than the same treatments given to older adults. Long-term follow-up clinical trials help identify these age-specific patterns.

Types of Long-Term Follow-Up Studies
Long-term follow-up clinical trials encompass various study designs that address different aspects of treatment safety and effectiveness over extended periods.
Active long-term follow-up clinical trials require ongoing participant involvement:
- Regular clinic visits for medical examinations and testing
- Periodic questionnaires about health status and quality of life
- Continued monitoring of specific organ functions or biomarkers
- Assessment of disease progression or treatment durability
- Documentation of new health conditions or treatments
Passive long-term follow-up clinical trials use existing medical records and databases:
- Electronic health record reviews to track major health events
- Cancer registry searches to identify new malignancies
- Insurance database analysis to detect healthcare utilization patterns
- Death certificate reviews to understand long-term mortality patterns
- Linkage with government health databases for comprehensive tracking
Registry-based long-term follow-up clinical trials create permanent databases that can follow participants indefinitely. These registries maintain contact with participants through regular updates and can quickly identify patterns when concerns arise.
Epidemiological long-term follow-up clinical trials use population-based approaches to study large groups of people who received specific treatments. These studies can detect rare long-term effects by analyzing data from thousands or tens of thousands of participants.
Biobank studies collect and store biological samples during long-term follow-up clinical trials. These samples allow future testing as new laboratory techniques develop or when specific safety questions arise years later.

Regulatory Requirements and Guidelines
Long-term follow-up clinical trials operate under specific regulatory frameworks that balance participant safety with practical considerations about extended research commitments.
The FDA provides guidance on when long-term follow-up clinical trials are necessary based on treatment characteristics and potential risks. Treatments that modify the immune system, affect genetic material, or have theoretical risks for delayed effects typically require extended monitoring.
Regulatory factors that influence long-term follow-up clinical trials requirements:
- Novel mechanisms of action with unknown long-term consequences
- First-in-class treatments without established safety profiles
- Treatments targeting children or young adults with decades of remaining life
- Irreversible treatments like gene therapy or certain surgical procedures
- Treatments with known delayed effects in animal studies
International guidelines help harmonize long-term follow-up clinical trials requirements across different countries. The International Conference on Harmonization provides standards that facilitate global research while ensuring consistent safety monitoring.
Ethics committee oversight continues throughout long-term follow-up clinical trials to ensure that extended monitoring remains justified and beneficial. These committees regularly review whether continued follow-up is providing valuable safety information.
Informed consent for long-term follow-up clinical trials must clearly explain the duration and nature of extended monitoring. Participants need to understand what long-term commitment they’re making when joining studies with follow-up requirements.

Duration and Intensity of Monitoring
Long-term follow-up clinical trials vary significantly in duration and intensity depending on the treatments being studied and the types of effects being monitored.
Common follow-up durations for different treatment types:
- Cancer treatments: 10-15 years to monitor for second cancers and late effects
- Gene therapies: 15-30 years due to permanent genetic modifications
- Immunotherapies: 5-10 years to track immune system changes
- Medical devices: Device lifespan plus 2-5 years for delayed complications
- Pediatric treatments: Until participants reach adulthood, plus additional years
Early years of long-term follow-up clinical trials typically involve more intensive monitoring with frequent visits and comprehensive testing. As time progresses and safety profiles become established, monitoring may transition to annual visits or periodic questionnaires.
Technology has transformed how long-term follow-up clinical trials collect information. Smartphone apps, wearable devices, and telemedicine platforms enable continuous monitoring without requiring frequent clinic visits. Electronic patient-reported outcome systems allow participants to report health changes in real-time.
Risk-based monitoring adjusts the intensity of long-term follow-up clinical trials based on emerging safety signals. If concerning patterns emerge, monitoring may become more frequent or comprehensive. Conversely, if treatments show excellent long-term safety, monitoring requirements may be reduced.
Geographic mobility presents challenges for long-term follow-up clinical trials as participants move to different cities or countries over time. Research networks and coordinated databases help maintain contact and continue monitoring regardless of location changes.

Participant Experience and Commitment
Long-term follow-up clinical trials require sustained commitment from participants who must balance ongoing research obligations with their changing life circumstances over years or decades.
The participant experience in long-term follow-up clinical trials evolves as people move through different life stages. Young adults may start families, change careers, or relocate for education. Older participants may develop new health conditions or face mobility challenges. Study designs must accommodate these natural life changes.
Common experiences during long-term follow-up clinical trials include:
- Annual or bi-annual clinic visits for comprehensive health assessments
- Periodic contact from research coordinators checking on health status
- Completion of detailed questionnaires about new symptoms or health changes
- Coordination with personal physicians to share relevant health information
- Participation in special studies if specific safety signals emerge
Communication strategies for long-term follow-up clinical trials must maintain engagement while respecting participants’ time and privacy. Regular newsletters about study progress help participants understand how their continued involvement contributes to medical knowledge.
Compensation for long-term follow-up clinical trials typically covers time and travel expenses for periodic visits. Some studies provide annual payments to acknowledge participants’ ongoing commitment to extended monitoring.
Life changes may affect participants’ ability to continue in long-term follow-up clinical trials. Research teams work flexibly to accommodate moves, schedule changes, or health issues that make clinic visits difficult. Remote monitoring options increasingly allow continued participation despite geographic or mobility barriers.

Data Management and Analysis
Long-term follow-up clinical trials generate massive amounts of data collected over many years from large numbers of participants. Managing and analyzing this information requires sophisticated systems and statistical approaches.
Database design for long-term follow-up clinical trials must accommodate decades of data collection while maintaining data quality and security. These systems need regular updates as technology evolves and must ensure that historical data remains accessible and analyzable.
Key data management challenges include:
- Maintaining data quality and consistency over extended time periods
- Integrating information from multiple sources and healthcare systems
- Protecting participant privacy while enabling important research
- Adapting to changing technology platforms and data standards
- Ensuring data remains accessible as staff and systems change
Statistical analysis of long-term follow-up clinical trials requires specialized methods that account for extended observation periods, varying follow-up durations, and missing data from participants who discontinue monitoring.
Signal detection algorithms continuously monitor long-term follow-up clinical trial data for patterns that might indicate safety concerns. These automated systems can identify unusual clusters of adverse events or unexpected trends in health outcomes.
Data sharing arrangements increasingly allow pooling of long-term follow-up clinical trials data across multiple studies and sponsors. These collaborative approaches provide larger sample sizes for detecting rare long-term effects and enable more comprehensive safety analysis.
Impact on Medical Practice
Long-term follow-up clinical trials have profoundly influenced medical practice by identifying delayed treatment effects that changed how therapies are used and monitored in clinical care.
Historical examples demonstrate the importance of long-term follow-up clinical trials in protecting patient safety. Studies of diethylstilbestrol (DES) revealed increased cancer risks in daughters of women who took this medication during pregnancy, but only through decades of follow-up. Similar long-term studies identified delayed cardiac effects of certain cancer chemotherapies.
Long-term follow-up clinical trials have led to important medical advances:
- Recognition of late effects from childhood cancer treatments
- Understanding of long-term cardiovascular risks from certain medications
- Identification of delayed benefits from treatments that prevent future disease
- Development of survivorship care guidelines based on long-term outcome data
- Optimization of treatment protocols to minimize long-term complications
Medical education now emphasizes the importance of considering long-term treatment effects when making clinical decisions. Long-term follow-up clinical trials data inform treatment guidelines and help physicians counsel patients about potential delayed benefits and risks.
Insurance coverage decisions increasingly consider long-term follow-up clinical trials data when evaluating treatment value. Evidence about long-term outcomes helps payers understand the full cost-effectiveness of medical interventions over time.
Patient advocacy organizations use long-term follow-up clinical trials data to support research funding priorities and influence treatment development. These organizations help ensure that long-term safety monitoring addresses patient concerns and priorities.
Technology and Innovation
Long-term follow-up clinical trials increasingly leverage technological innovations that make extended monitoring more efficient and participant-friendly while improving data quality and completeness.
Electronic health record integration allows long-term follow-up clinical trials to access routine medical care data without requiring additional participant visits. These systems can automatically identify hospitalizations, new diagnoses, or prescription changes relevant to safety monitoring.
Technological advances improving long-term follow-up clinical trials include:
- Wearable devices that continuously monitor vital signs and activity patterns
- Smartphone apps that collect patient-reported outcomes in real-time
- Telemedicine platforms that enable remote clinical assessments
- Artificial intelligence systems that analyze complex longitudinal data
- Blockchain technologies that ensure data security while enabling sharing
Mobile health technologies enable continuous monitoring between formal study visits. Participants can report symptoms, track medications, and provide health updates through user-friendly applications that integrate with study databases.
Predictive analytics help identify participants at high risk for specific long-term effects, enabling targeted monitoring that focuses resources where they’re most needed. These approaches improve efficiency while maintaining comprehensive safety oversight.
Virtual reality and gaming technologies are being explored to maintain participant engagement during long-term follow-up clinical trials. These innovative approaches recognize that sustained participation over years or decades requires creative engagement strategies.
At Valiance Clinical Research, we recognize that long-term follow-up clinical trials represent a profound commitment between researchers and participants. Our community-based approach ensures that extended monitoring remains accessible and convenient for diverse populations across our 6 Southern California locations.
Our 70% diverse enrollment and 95%+ retention rates reflect our dedication to maintaining long-term relationships with participants who contribute to extended safety monitoring. We understand that long-term follow-up clinical trials require trust, flexibility, and ongoing support to succeed.
Conclusion
Long-term follow-up clinical trials demonstrate the medical research community’s commitment to participant safety that extends far beyond active treatment periods. These studies represent a promise to monitor your health and contribute to medical knowledge that protects future patients for years or decades to come.
Understanding long-term follow-up clinical trials helps you appreciate the comprehensive safety framework that surrounds clinical research participation. Your commitment to extended monitoring contributes to the ongoing refinement of medical treatments and the prevention of delayed adverse effects.
Consider the long-term follow-up commitment when evaluating clinical trial participation. While these requirements represent additional time and effort, they provide ongoing medical monitoring and contribute to medical knowledge that benefits countless others facing similar health challenges.
Contact Valiance Clinical Research to learn about clinical trials with long-term follow-up requirements and how we support participants through extended monitoring periods. We explain what long-term commitment involves and help you understand how your continued participation contributes to advancing medical safety for everyone.